Introduction
Rising prescription drug spending continues to drive health care costs in Massachusetts and the U.S. In 2017, total prescription drug spending at pharmacies grew 4.1% in Massachusetts, net of additional manufacturer rebates and discounts, representing one of the highest growth sectors of health care spending in the state. [1] MassHealth prescription drug spending nearly doubled in five years, from $1.1 billion in 2012 to $1.9 billion in 2017, growing twice as fast as other MassHealth spending. [2]
Pharmacy benefit managers (PBMs) manage prescription drug benefits for many health plans and negotiate prices and rebates with manufacturers and payments to pharmacies. Their practices have increasingly raised concerns based on a lack of transparency and potential contributions to high drug costs. In particular, the industry now faces scrutiny for using the practice known as “spread pricing” for generic drugs, in which the PBM charges payers more for a drug than it reimburses the pharmacy that dispensed the drug and keeps the difference as potential profit. PBM use of spread pricing appears to be increasing: this practice covered 22% of PBM compensation in 2014, but rose to 54% in 2016. [3] This practice, often used as a means of payment for PBM services instead of administrative fees, may have significant impacts on public insurance programs, employer health plans, and consumers. Additionally, the media has reported growing concerns from pharmacists about low reimbursement rates from PBMs in Massachusetts and other states. [4,5,6] PBM payments to pharmacies are sometimes even below the pharmacy’s acquisition costs of the drugs, which can affect the financial viability of pharmacies and potentially impact access to care. Yet the extent to which PBMs profit from this practice, and on which drugs, remains largely hidden from payers and the public.
As part of the fiscal year 2020 state budget strategy on MassHealth drug prices, the Baker-Polito administration proposed a new requirement for PBMs to be transparent about their pricing and to limit PBM margins under contracts with MCOs and accountable care organizations (ACOs), which the administration projects will save $10 million. [7] To advance transparency, MassHealth recently released a bulletin directing MCOs and MassHealth Accountable Care Partnership Plans to obtain and submit to MassHealth drug-specific data from their PBMs including payments to dispensing pharmacies and rebate and administrative payment data. [8] The HPC’s 2018 Cost Trends Report similarly recommended that the Commonwealth should increase state oversight of PBM pricing and take steps to limit the practice of “spread pricing.” [9] To further investigate this practice and its impact in Massachusetts, this twelfth issue of HPC DataPoints contains new data on PBM pricing for generic drugs in the Massachusetts Medicaid and commercial market.
Spread Pricing Model
Below is an illustration of spread pricing using hypothetical prices. The price spread refers to the difference between what the PBM reimburses the pharmacy for a drug and what it charges the payer – the PBM retains the difference as potential profit. This model stands in contrast to a “pass-through” model, in which PBMs charge payers the same amount that they reimburse pharmacies, plus an administrative fee.
The Centers for Medicare & Medicaid Services (CMS) requires Medicaid Fee-For-Service (FFS) programs to use a transparent pass-through model, mandating that all state FFS programs reimburse pharmacies based on the acquisition cost of the drug plus a set dispensing fee, a policy that went into effect on April 1, 2017. In Massachusetts, MassHealth FFS’ reimbursement formula for most drugs is the drug acquisition cost plus a professional dispensing fee of $10.02.[10, i]
CMS’ requirements for the Medicaid FFS program do not apply to Medicaid Managed Care Organizations (MCOs). Therefore, PBMs are currently permitted to use spread pricing in contracts with MassHealth MCOs. The lack of transparency in PBM payment arrangements makes it difficult for payers such as MassHealth MCOs to determine the value of their drug spending and how payments are distributed.
The below interactive graphics display best in full screen mode. To view them in full screen, scroll to the bottom of each graphic and click on the far-right icon. Use the same icon to return to the original view. These controls work best in Internet Explorer.
Methods
This analysis examines PBM pricing practices for generic drugs in the MassHealth MCO program and the commercial market. First, we compared MassHealth MCO prices to FFS prices for drugs reimbursed by both programs. While operational factors such as differences in contract terms and fluctuating acquisition costs can impact differentials, the FFS prices based on a pass-through model represent a benchmark to evaluate PBM prices in the MCO program. For commercial payers, we compared the payer price for a given generic drug to the pharmacy acquisition cost for the drug, based on the National Average Drug Acquisition Cost (NADAC). The difference between the two is largely comprised of the dispensing fee to pharmacies and the potential profit kept by PBMs. Since there are no publicly available data on PBM reimbursement rates to pharmacies, these methods represent only an approximate indication of how large PBM profits may be on generic drugs.
Price Differences for Generic Drugs Between the Masshealth FFS and MCO Programs
In 2018 Q4, the latest time period for which Medicaid data are available, MCO prices were higher than NADAC acquisition prices for 95% of the unique drugs analyzed, but MCO prices were higher than FFS prices for only 42% of unique drugs. FFS payments use a formula based on an acquisition price measure and a $10.02 pharmacy dispensing fee. Whether the MCO price is higher or lower than the FFS price, it is unclear how much of the payment the PBMs apportion to reimbursing the pharmacy for its costs and how much is retained as PBM profit.
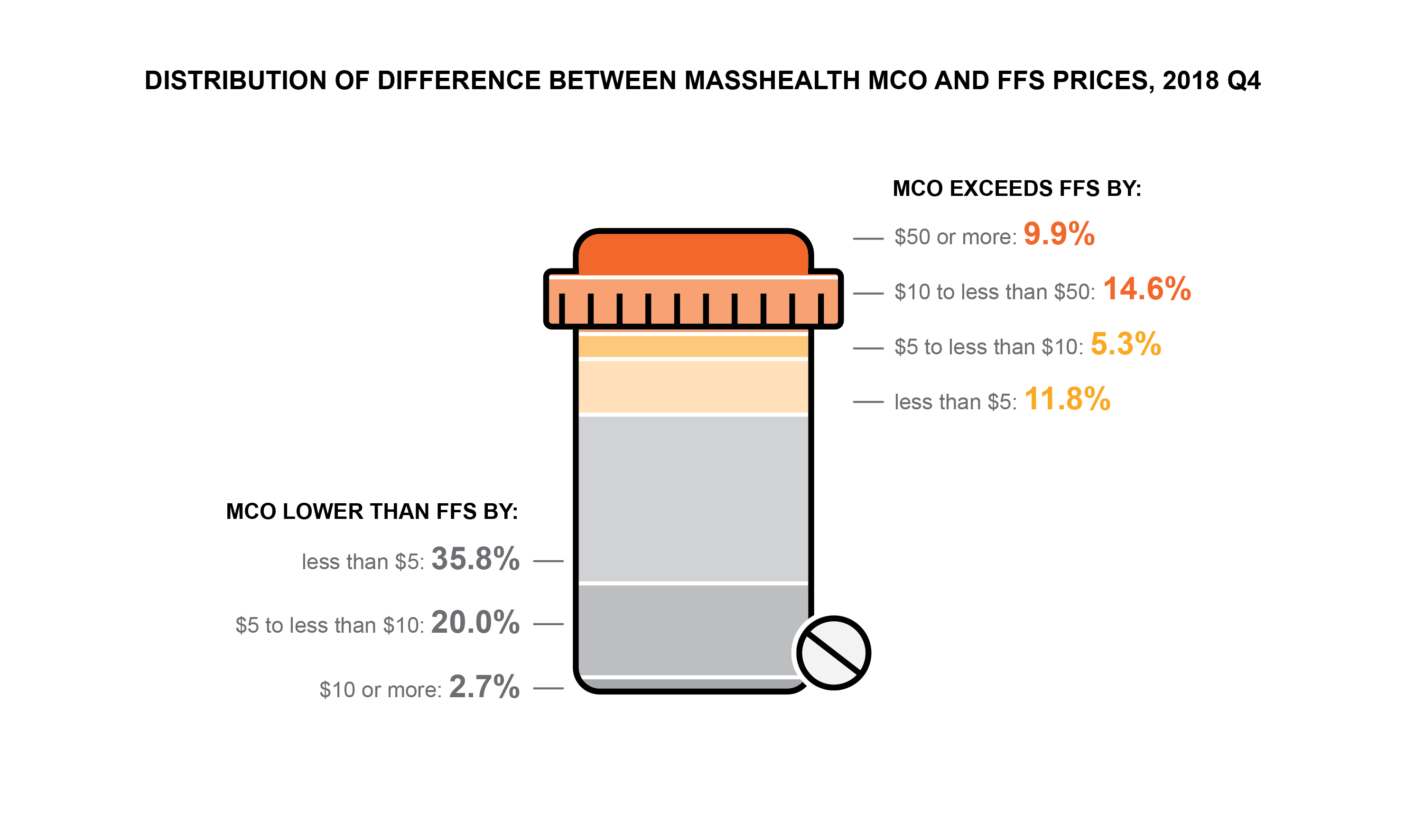
Furthermore, for those drugs where MCOs paid a higher price than FFS, the difference was often substantial, leading to higher average drug prices overall. MCO prices exceeded FFS prices by an average $15.97 per unique drug, despite being below FFS prices for more than half (58%) of unique drugs. [ii] As shown below, the MCO price exceeded the FFS price by at least $10 for nearly 25% of unique drugs and was at least $50 higher for approximately 10% of unique drugs.
Higher generic drug prices paid by MCOs come out of the fixed per-member (capitation) payment rate from MassHealth to cover a beneficiary’s medical and pharmacy benefits. Therefore, while higher drug prices do not necessarily translate to direct state spending in the short term, these prices can lead to MCOs allocating fewer resources for other medical services and can raise spending in the long term through higher capitated rates. On the other hand, lower MCO prices could indicate low PBM reimbursement rates to pharmacies, which could lead to falling margins at pharmacies, particularly those that serve a high proportion of Medicaid MCO beneficiaries.
Top Generic Drugs by Price Differential
The figure below shows the generic drugs with the largest differences between MCO and FFS prices per prescription in 2018 Q4. For example, the price per prescription of the antiviral medication Valganciclovir 450 mg tablets (generic Valcyte) was on average $1,134 higher for MCOs than FFS.
Cumulatively, the differences per prescription add up to significant spending. The figure below shows the top 20 generic drugs by aggregate spending difference (MCO price difference over FFS per prescription, multiplied by the volume of prescriptions in MCOs). Notably, Buprenorphine-Naloxone 8-2 mg (generic Suboxone) – a drug used to treat opioid use disorder and a critical component of the state’s strategy to address the opioid crisis – had the highest aggregate spending difference in 2018 Q4, totaling $252,536.
In 2018 Q4, MCOs paid an average $159.24 per prescription of Buprenorphine-Naloxone 8-2 mg, 111% higher than the average FFS price of $75.53. [iii] While this difference of $83.70 did not place Buprenorphine-Naloxone in the top 20 drugs by difference per prescription, the high utilization of the drug led to its rank as highest total difference for MCOs.
The finding of high prices on Buprenorphine-Naloxone is particularly striking because average acquisition cost for Buprenorphine-Naloxone 8-2 mg SL tablets has been falling steadily, while the price Massachusetts Medicaid MCOs paid for this drug has not decreased in tandem. From 2016 Q1 to 2018 Q4, average acquisition cost for Buprenorphine-Naloxone 8-2 mg SL tablet [iv] fell by 60% while the MassHealth MCO price increased by 13%. The visualization below shows several widely-prescribed generic drugs where a drop in acquisition cost has not translated to lower prices for the MassHealth MCO program.
PBM Pricing for Generic Drugs in the Commercial Market
In the commercial market, the HPC also observed PBM prices for generic drugs that were dramatically higher than the drugs’ acquisition costs, shown in figures below, based on data from the fourth quarter (Q4) of 2016, the most recent available commercial pharmacy claims data in the All-Payer Claims Database. Comparing average pharmacy acquisition costs to average commercial prices, we found Imatinib mesylate 400 mg tablets (generic Gleevec, used in treatment of leukemia) had among the highest average differentials per prescription of $1,811 above the pharmacy’s acquisition cost, which translated to $278,937 in aggregate spending above acquisition cost in 2016 Q4.
State Activity
Massachusetts and a number of other states are pursuing action to increase oversight of PBMs to ensure that public dollars are spent efficiently at all points in the drug distribution chain. A number of states have introduced legislation requiring PBMs to be licensed by the state and to disclose information on pricing, rebates, and reimbursement to pharmacies, among other actions. [6, 11, 12]
In August 2018, Ohio announced that its Medicaid MCO programs would end their spread pricing contracts with PBMs and switch to a pass-through model following a state audit that found PBM profit accounted for 31.4% ($208.4 million) of the $662.7 million paid by Ohio Medicaid MCOs for generic drugs. [13] Additionally, the audit found that PBM cuts to Medicaid reimbursements to pharmacies coincided with a large number of pharmacy closures in the state. [v]
PBMs assert that spread pricing models provide more predictability for health plans than pass-through models, in which drug prices for plans fluctuate directly with changes in drug acquisition cost. However, with greater transparency, payers can make informed choices about allocation of state spending or premium dollars, including appropriate compensation for both pharmacies and PBMs. While this analysis does not provide estimates of PBM margins from drug pricing, the results suggest that opportunities to lower drug spending through more transparent PBM practices exist for both public and commercial payers in Massachusetts.
References
[1] Center for Health Information and Analysis. Performance of the Massachusetts Health Care System, Annual Report. Sept. 2018. Available at: http://www.chiamass.gov/annual-report/
[2] Executive Office of Health and Human Services. MassHealth Prescription Drug Pricing FY20 H.1 Proposal. Jan. 23, 2019. Available at: https://www.mass.gov/files/documents/2019/01/23/masshealth-prescription-drug-pricing-proposal-FY20.pdf
[3] Fein A. 2017 Economic Report on U.S. Pharmacies and Pharmacy Benefit Managers. Drug Channels Institute. Feb., 2017. Available at: http://drugchannelsinstitute.com/files/2017-PharmacyPBM-DCI-Overview.pdf
[4] Langreth R, Ingold D, Gu J. The Secret Drug Pricing System Middlemen Use to Rake in Millions. Bloomberg. Sep. 11, 2018. Available at: https://www.bloomberg.com/graphics/2018-drug-spread-pricing/
[5] Morelli J. Prescription Drug Pricing Strategy: Where is the Money Going? Boston 25 News. Jan. 14, 2019. Available at: https://www.boston25news.com/news/prescription-pricing-strategy-where-is-the-money-going-/903919305
[6] Dunn C. PA Auditor General Wants to Take a Whack at Firms that Negotiate Drug Benefits for the Medicaid Program. The Inquirer. Dec. 11, 2018. Available at: http://www.philly.com/business/pbms-pennsylvania-medicaid-drug-prices-cvs-auditor-general-20181211.html
[7] Commonwealth of Massachusetts. The Governor’s Budget Recommendation. Fiscal Year 2020 House 1. Jan. 23, 2019. Available at: https://budget.digital.mass.gov/bb/h1/fy20h1/dnld_20/fy2020h1.pdf
[8] Executive Office of Health and Human Services. MassHealth Managed Care Entity Bulletin 11. Apr. 2019. Available at: https://www.mass.gov/files/documents/2019/04/11/mce-11.pdf
[9] Massachusetts Health Policy Commission. 2018 Cost Trends Report. Feb. 2019. Available at: https://www.mass.gov/doc/2018-report-on-health-care-cost-trends
[10] U.S. Department of Health and Human Services. Medicaid Covered Outpatient Prescription Drug Reimbursement Information by State: Quarter Ending December 2018. Available at: https://www.medicaid.gov/medicaid/prescription-drugs/state-prescription-drug-resources/drug-reimbursement-information/index.html
[11] National Academy for State Health Policy Center for State Rx Drug Pricing. Comparison of State Pharmacy Benefit Manager Laws. Available at: https://nashp.org/comparison-state-pharmacy-benefit-managers-laws/
[12] Bai G, Socal MP, Sharp M, et al. Medicaid Manager Care Programs’ Contracts For Generic Drugs Are Inefficient. Health Affairs Blog. May 1, 2019. Available at: https://www.healthaffairs.org/do/10.1377/hblog20190426.775617/full/?utm_source=Newsletter&utm_medium=email&utm_content=Washington+State+s+Public+Option+1+0%3B+The+Lancet+Commission+on+Global+Health+Law%3B+Medicaid+Managed+Care+Contracts+For+Generic+Drugs&utm_campaign=HAT+5-1-19
[13] Ohio Auditor of State. Ohio’s Medicaid Managed Care Pharmacy Services. Aug. 16, 2018. Available at: https://audits.ohioauditor.gov/Reports/AuditReports/2018/Medicaid_Pharmacy_Services_2018_Franklin.pdf
Notes
[i] MassHealth FFS generally sets drug prices as the lower of NADAC plus a $10.02 professional dispensing fee or Usual and Customary (U&C) prices. In case of unavailability of NADAC, the wholesale acquisition cost (WAC) plus a $10.02 professional dispensing fee is used to compare to U&C.
[ii] The analysis pools drugs with the same dosage form and dosage strength, but different package sizes, into the same unique drug. The average price per prescription does not factor the number of prescriptions per unique drug.
[iii] Prices per prescription model a standard number of units per prescription.
[iv] NDC 00054018913
[v] Reports from 46Brooklyn estimate that PBM payments to Ohio pharmacies resulted in an average pharmacy margin of $1.15 per prescription, far lower than the dispensing fee of $10.49 that Ohio pharmacies estimate is required to break even. Source: https://www.46brooklyn.com/research/2018/9/13/bloomberg-puts-drug-price-markups-on-the-map
Additional Resources
Contact for HPC DataPoints, Issue 12: Cracking Open the Black Box of Pharmacy Benefit Managers
Online
Phone
HPC-Info@state.ma.us
Address
| Date published: | June 5, 2019 |
|---|