CP Composition
i. Description of Affiliated Partners that comprise Boston Allied Partners. Boston Allied Partners (BAP) brings over 40 years of experience in home-based care services and supports for children and adults ages 3 to 64 that are part of MassHealth and have long term services and supports (LTSS) needs. BAP is a partnership of Boston Medical Center (BMC) and the three Aging Services Access Points (ASAPs) that serve the Boston area: Boston Senior Home Care, Central Boston Elder Services, and Ethos. The ASAPs that serve Boston provides direct services to older adults, including information and referral; interdisciplinary case management: intake, assessment, development and implementation of service plans; monitoring of service plans; and reassessment of needs; and investigations of abuse and neglect of elders. Collectively, our aging service providers and BMC currently care for over 33,000 people across Boston annually.
BAP’s team speaks over 20 languages and is focused on providing culturally sensitive engagement and care to meet the needs of individuals with Complex LTSS needs; Brain injury or cognitive impairments; Physical disabilities; and/or Intellectual disabilities and developmental disabilities including autism. In addition, BAP has provided care for patients enrolled in a variety of provider networks including accountable care organizations, managed care organizations, Senior Care Options (SCO) and One Care programs.
Community Partners Population Served
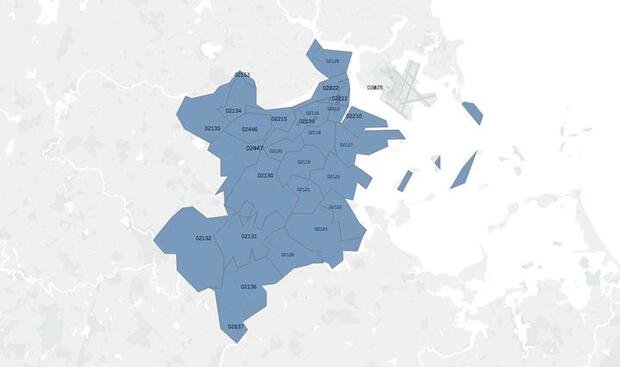
i. Service Area list. BAP is responsible for covering the Boston Primary Service area, which includes all neighborhoods in the city of Boston as well as the city of Brookline.
ii. Demographics of BAP population served. Boston Allied Partners serves patients in the Boston Primary Area. We have extensive expertise serving children and youth (ages 3 to 21) and adults (ages 22 to 64) with LTSS needs, and addressing social determinants of health. We are also experienced in assisting individuals with brain injuries or cognitive impairments, individuals with physical disabilities, individuals with Intellectual Disabilities and Developmental Disabilities (I/DD) and older adults (up to age 64) with LTSS needs to keep them as healthy and engaged in their communities for as long as possible.
Although most children and youth with LTSS needs will be served by BMC, our partners also have experience with the population ages 16 to 21. BAP plans to leverage this experience as we help transition high need pediatric patients to adult services.
Overview of 5-Year Business Plan
i. Long term goals.
1. Technology and information sharing. BAP’s technology and information sharing goal is to develop on-demand dashboards using our technology platform that can be shared with ACO/MCO partners, indicating what social services members have been connected to, with what frequency and with the ability to segment the population to provide deeper insights into what impacts quality/cost and what may not. We will be collaborating with our technology platform, ACT.md, to provide enhanced feedback to our contracted partners, including what connections to community resources we have provided and how many of each type of community resource across the population. We also hope to provide feedback about the specific providers/social service agencies that their members are choosing for their care. These reports will be built manually at first, with the intention of automating them throughout the duration of the project.
Our technology system also has the capacity to include community members, therefore the longer term application is continued contact amongst the LTSS workforce and community connections beyond the medical teams. The continued contact will establish local connections and supports that will enhance health outcomes. In addition, BAP Care Coordinators will be trained to identify and access key community-based LTSS resources while working with Aunt Bertha to develop a library of preferred social service agencies and LTSS providers for each ACO/MCO in order to connect members to service agencies who have developed expertise in treating this population. Overall this level of information sharing will improve member experience, continuity of care, and quality of care by holistically engaging our patient population.
2. Workforce development. BAP will train staff to successfully co-navigate the ACO/MCO landscape with ACO/MCO care teams and comprehensively assess the social determinants of health of Enrollees using eight different domains of questions including housing instability, food insecurity, energy insecurity, transportation problems, medication costs challenges, education needs, employment needs and caregiving needs. In addition, BAP will use Community Health 3 Worker (CHW) Registration certification programs that are available for staff through the Commonwealth, take advantage of the trainings being offered through the Statewide Investments initiative for all staff, and hold ongoing trainings and continuing education sessions. Our long term goals are to: (1) increase staff retention and engagement of our frontline staff and (2) build a workforce that sets the benchmark nationally for having the best strategies for identifying and removing the barriers to resolving social determinants of health such as housing and homelessness.
3. Program administration. At present, our program administration goal is to not receive any zero achievement points for any measures. If so, we will focus improvement efforts on those measures in the following quarter/year. Prior to establishment of our Quality Management Committee (expected to first convene in July/August 2018), we will be focused on member engagement, specifically the number of members with a completed LTSS Care Plan in 90 days (EOHHS Anticipated LTSS CP Quality Measure Slate, part V, #10) will be the target (EOHHS specifies that the target should be 70% or above).
ii. Anticipated challenges. We anticipate challenges in three main areas: technology and information sharing, workforce development, and program administration. For technology and information sharing, we expect that the technology build itself will take longer than we expect and that it may take time to work out all of the bugs in the platform. Therefore we anticipate that there may be multiple iterations of the platform before we are up and running. In terms of workforce development, we believe that recruitment and retention be challenging for this program as we want to hire linguistically and culturally competent staff to the best of our ability. Lastly we anticipate program administration challenges surrounding the Quality Measures as we work to continuously improve from previous scores. If we at any point receive zero achievement points or a low score for any measures, we will focus our efforts on maintaining a better score in the near future.
In addition, as part of a demonstration project, we expect there to be challenges in continued operations of the program since we will be building and learning at the same time. With particular respect to the composition of BAP, we do expect that we will be receiving a disproportionate share of pediatric referrals from ACO/MCO partners in the Boston Primary Area. Once we reach capacity, we anticipate challenges in finding alternate service facilitators for this population. Over the longer term, we hope to address this challenge in partnership with EOHHS in hopes of adjusting our model to accommodate the increased numbers, should this concern be realized.
iii. Sustainability. Each of our ACO partners has very different business models and many are approaching our partnerships very differently. In order to be most efficient in delivering LTSSrelated supports for our patients, we will need to have a good understanding of the existing ACO/MCO structures and what supports they have built expertise in. For example, if we have many patients from a particular ACO/MCO on our panel who have been connected with services 4 and have only connections to a food bank outstanding and that ACO/MCO partner has a food bank on-site, we would want to know that in order to graduate those patients and take on other high-need individuals. While this seems intuitive, we anticipate that this will take time as we build trust with our partners.
We anticipate refining our outreach model over time to increase expertise and efficiencies. The goal is to become an embedded resource to each ACO/MCO and continue our ACO/MCO business relationship past the five year demonstration. Throughout the course of these 5 years, we will be paying extra attention to operational inefficiencies amongst organizations in order to successfully alleviate the need for an ACO/MCO to develop in-house LTSS support structures.
Additional Resources
-
Open PDF file, 318.42 KB, Boston Allied Partners (English, PDF 318.42 KB)