Central Processing Unit
The Central Processing Unit (CPU) received 5,369 new referrals for investigation in fiscal year 2019 (FY19) from the following sources.
Table 2. FY19 CPU Referral Sources
|
Source |
Number of Referrals |
Percentage of Total |
|---|---|---|
|
Department of Transitional Assistance |
3,444 |
64.1% |
|
MassHealth |
1,218 |
22.7% |
|
Hotline |
571 |
10.6% |
|
Data Analytics Unit |
78 |
1.5% |
|
Task Force |
38 |
0.7% |
|
Department of Early Education and Care |
14 |
0.3% |
|
Other |
6 |
0.1% |
The following is a breakdown of the public assistance programs involved in the 5,369 new referrals.
Table 3. FY19 CPU Caseload by Public Assistance Program
|
Type |
Number of Cases |
Percentage of Total* |
|---|---|---|
|
Supplemental Nutrition Assistance Program |
2,240 |
44.2% |
|
MassHealth |
1,562 |
24.8% |
|
Transitional Aid to Families with Dependent Children |
1,051 |
17.1% |
|
Emergency Aid to the Elderly, Disabled and Children |
469 |
13.2% |
|
Other |
29 |
0.5% |
|
Classification to Be Determined |
18 |
0.1% |
*Percentages do not total 100 due to rounding.
In FY19, CPU processed, analyzed, and reviewed 5,181 referrals. CPU team members identified 791 referrals as potential intentional program violation (IPV) cases, where BSI determined that a fraud claim had merit but returned the case to the Department of Transitional Assistance (DTA) for further action based on the evidence. Typical agency actions include civil recovery, disqualification, and recalculation of benefits. Additionally, CPU closed 3,188 referrals administratively with no fraud determined after completing a preliminary investigation. CPU designated 1,202 referrals for case assignment. CPU team members continued to carry a small caseload in FY19. The unit completed 279 DTA cases, identifying fraud in 248 cases.
Department of Transitional Assistance Unit
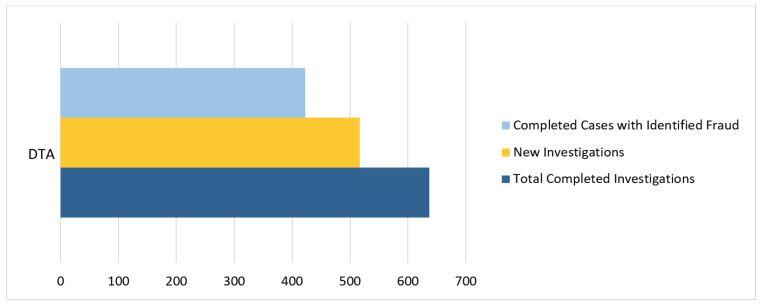
The DTA Unit was assigned 517 new cases in FY19, completed 637 cases, and identified fraud totaling $5,950,080.24 in 423 cases. The DTA Unit’s breakdown of identified fraud by public benefit program was as follows: $3,893,806.05 for Supplemental Nutrition Assistance Program (SNAP) investigations (33%); $1,223,408.12 for Transitional Aid to Families with Dependent Children (TAFDC) investigations (10%); and $395,525.24 for Emergency Aid to the Elderly, Disabled and Children (EAEDC) investigations (3%).
In FY19, the DTA Unit filed criminal charges in 18 cases in various courts throughout the Commonwealth. One case resulted in an indictment in US District Court, while 17 cases were charged in district courts.
Figure 8. FY19 DTA Caseload
Note: BSI’s DTA caseload for FY19 included SNAP, TAFDC, and EAEDC cases.
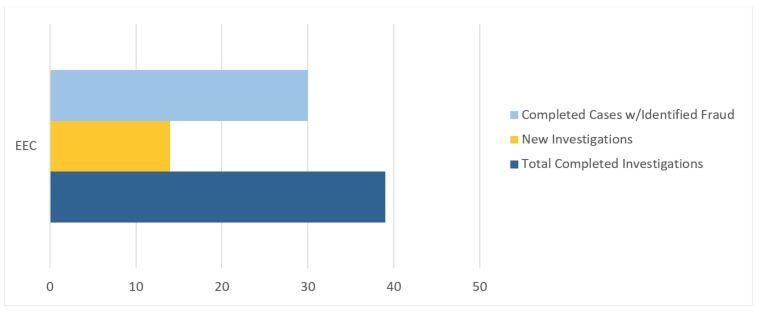
In addition, the DTA Unit received 14 referrals from the Department of Early Education and Care (EEC) and identified $1,401,578.69 in fraud from these referrals. As part of BSI’s continued working relationship with EEC, EEC’s designated financial assistance worker liaison with BSI is able to efficiently track and assist with BSI’s EEC caseload and provide much-needed documentation and information in an expedited manner for speedier investigations.
Because individuals suspected of defrauding EEC often also receive other forms of public assistance, BSI routinely checks EEC subjects’ other public assistance benefits and, in particular, their reporting of household income and composition to other agencies. These supplemental investigations have led to the discovery of additional fraud in DTA and MassHealth public benefit programs.
Figure 9. FY19 EEC Caseload
DTA also conducted 54 civil recoveries in FY19. In those cases, subjects had the opportunity to enter into repayment agreements with DTA and/or EEC. In FY19, BSI initiated repayment agreements and disqualification consent agreements (DCAs) totaling $1,459,347.84. DCAs are agreements subjects sign to disqualify themselves from receiving further DTA and/or EEC benefits because of their IPVs. When pursuing civil recovery for DTA and EEC cases, BSI requires DCAs rather than administrative hearings.
MassHealth Unit
During FY19, the MassHealth Unit was assigned 419 new cases, completed 631 cases, and identified fraud totaling $2,796,003.28 in 400 cases. In addition, the MassHealth Unit assisted the DTA Unit by completing 37 DTA/EEC cases with identified fraud totaling $754,031.16.
During FY19, the MassHealth Unit had four of its court cases resolved—three in district court and another in superior court. Two of the district court cases were in Quincy. In the first, a MassHealth recipient who resided out of state had her case continued without a finding for one (1) year and received an order to perform 100 hours of community service. In the second case, a MassHealth recipient received a guilty verdict on the charge of larceny under $250 and a sentence of 18 months’ probation for submitting falsified timesheets for personal care attendant (PCA) services after his PCA stopped working for him in 2015. The third district court case, in Pittsfield, resulted in another continuance without a finding. Unlike the prior two cases, however, the defendant in Pittsfield is required to repay full restitution—$14,946.47—within 18 months.
In FY19, the MassHealth Unit resumed its participation in the PCA Task Force in collaboration with the Attorney General’s Office and federal Inspector General’s Office of Investigations. Two BSI supervising fraud examiners and a senior fraud examiner are currently representing BSI on the task force. During FY19, 426 cases included PCA-related fraud allegations and 297 of those cases had identified fraud, totaling $866,172.81.
Figure 10. FY19 MassHealth Caseload
In FY19, the MassHealth Unit conducted 31 civil recoveries, in which subjects entered into repayment agreements with MassHealth, totaling $468,144.67.
Data Analytics Unit
The growth of BSI’s DAU, its increasing technical capabilities, and its continued collaboration with partners led to 71 referrals to CPU. The majority of the CPU referrals alleged that PCAs falsely submitted timesheets for services to MassHealth members in long-term care facilities and PCAs were not reporting income earned as PCAs to DTA as required while receiving public assistance benefits.
BSI examiners completed 215 DAU-generated referrals that carried into FY19. These referrals also related to the improper submission of timesheets by PCAs, and 208 referrals were completed with identified fraud. DAU also continued to field referrals from BSI’s Public Assistance Fraud Hotline. DAU received and analyzed 10 referrals made through the hotline alleging provider fraud, five (5) of which remain ongoing.
In addition, using advanced data analysis, DAU was able to identify MassHealth providers with a high potential for fraud. DAU identified and referred eight (8) MassHealth providers, which consisted of 16 total healthcare entities. The analysis of these referrals focused on improper billing associated with a variety of healthcare providers and services, including, but not limited to, home health care, adult foster care, dermatological services, evaluation and management services, and the use of certain claim modifiers. DAU referred these findings to the Office of the State Auditor’s Medicaid Audit Unit.
DAU continues to support multiple state and federal partners through joint investigative work in addition to accepting referrals for investigation and creating and sending referrals to the appropriate entities. For example, DAU is collaborating with federal partners, including the federal Office of the Inspector General’s Office of Investigations and the Executive Office of Health and Human Services, on four (4) ongoing investigations related to services provided within both the Medicaid and Medicare programs.
During FY19, DAU assisted with the establishment of a standard operating procedure (SOP) between Audit Operations’ DAU, BSI’s DAU, and the Office of the State Auditor’s (OSA’s) Medicaid Audit Unit. The SOP facilitates cross-unit collaboration and ensures that the OSA is using its resources as efficiently and effectively as possible.
Lastly, DAU initiated the rollout of its analytical support services at the close of FY19. DAU will formally introduce these services in early FY20, when all services will be fully available. The goal is to aid BSI examiners in their investigations by outsourcing data analysis tasks to DAU. Support services will include the creation of charts, maps, timelines, or graphs needed for visual presentation; optical character recognition (OCR) services; social network analysis; general data analysis; and technical training.
| Date published: | January 22, 2020 |
|---|