Central Processing Unit
CPU received 5,062 new referrals for investigation in FY25 and processed, analyzed, and reviewed 3,990 referrals from the following sources.
Table 2. CPU Referral Sources for FY25
| Referral Source | Number of Referrals Processed, Analyzed, and Reviewed | Percentage of Total |
|---|---|---|
| DTA | 1,963 | 49% |
| Hotline | 1,198 | 30% |
| DAU | 768 | 19% |
| MassHealth | 37 | 1% |
| PCA Task Force | 23 | 1% |
| Law Enforcement | 1 | 0% |
The following is a breakdown of the public assistance programs involved in the 3,990 referrals processed, analyzed, and reviewed.
Table 3. CPU Caseload for FY25, by Public Assistance Program
| Case Type | Number of Cases | Percentage of Total |
|---|---|---|
| Supplemental Nutrition Assistance Program (SNAP) | 3,106 | 78% |
| MassHealth | 439 | 11% |
| Transitional Aid to Families with Dependent Children (TAFDC) | 246 | 6% |
| Emergency Aid to the Elderly, Disabled and Children (EAEDC) | 80 | 2% |
| Merge Case* | 60 | 2% |
| Other | 40 | 1% |
| PCA | 15 | 0% |
| EEC | 3 | 0% |
| Supplemental Security Income | 1 | 0% |
* Merge cases occur when BSI receives a separate allegation on a subject that is already under investigation. The new allegation is merged into the existing case for investigative and administrative purposes.
CPU staff members identified 1,323 referrals as potential IPV cases, for which BSI determined that a fraud allegation had merit but returned the case to DTA for further action based on the evidence. Typical agency actions include civil recovery, disqualification, and recalculation of benefits. Additionally, CPU closed and/or merged 1,873 referrals for which no fraud was identified after completing preliminary investigations. CPU designated 794 referrals for active investigation. In addition to processing, analyzing, and reviewing the referrals discussed above, CPU completed 48 investigations during this report’s FY.
During FY25, CPU assisted with DAU’s PCA High Earner Project. For this project, DAU analyzed PCA income provided by MassHealth for the highest-earning14 from this project. CPU processed, analyzed, reviewed, and made case recommendations for all these referred cases.
CPU staff members are in direct contact with the public and stakeholders. CPU manages referral intake calls and an online referral process—collectively categorized as hotline referrals. In FY25, CPU completed the intake process for 1,242 hotline referrals.15 Additionally, CPU regularly assists members of the public with issues involving their receipt of public benefit–related mail, or access to other state agencies. Although these issues fall outside of BSI’s statutory charge (i.e., investigating public benefit fraud), we help the public by directing individuals to the agencies best able to address their issues and respond to their questions.
CPU also communicates and collaborates as a team to assist examiners during their investigations. CPU uses various technical resources to stay current with guidelines and to verify allegations received. As a result, CPU continuously updated examiners throughout FY25 regarding any changes to both policy/income guidelines in connection with public benefit programs and other guidance from our stakeholders. These actions contributed to BSI’s successes in FY25.
Fraud Investigations Unit
FIU consists of a special investigator, eight fraud examiners, and one senior fraud examiner, all of whom are under the supervision of an assistant director and three supervising fraud examiners.
FIU completed 869 cases in FY25, which contributed to identifying fraud totaling $6,316,407 in 496 cases.
Table 4. FIU Identified Fraud during FY25, by Public Assistance Program
| Public Assistance Program | Identified Fraud |
|---|---|
| SNAP | $4,121,011 (65%) |
| MassHealth | $1,301,957 (21%) |
| TAFDC | $328,807 (5%) |
| Other/Task Force | $259,589 (4%) |
| PCA | $143,835 (2%) |
| Social Security Administration | $101,257 (2%) |
| EAEDC | $59,951 (1%) |
During FY25, FIU completed 22 civil recoveries, totaling $768,752 in fraudulent overpayments. The BSI civil recovery process begins with a reporting examiner contacting the subject and arranging a meeting—either in person or virtually. In cases where the subject agrees to repay the identified overpayment, they may execute a repayment agreement. Once an agreement is signed, the documents are forwarded to the appropriate agency to initiate collection.16 BSI does not have the statutory authority to collect or direct collection of overpayments.
In FY25, BSI continued to adhere to the May 2023 federal directive from the Centers for Medicare and Medicaid Services,17 which prohibits the collection of overpayments from recipients of Medicare and Medicaid services. As a result of this directive, BSI returns all completed MassHealth investigations that include financial findings back to MassHealth for documentation and recordkeeping. BSI works closely with the Medicaid Fraud Division of the Attorney General’s Office and the US Department of Health and Human Services’ Office of the Inspector General to investigate serious cases of PCA fraud. This collaborative group, called the PCA Task Force, meets regularly throughout the year to review case developments and coordinate next steps to ensure efficient case management. In FY25, BSI expanded its involvement by assigning additional examiners to participate in PCA Task Force investigations. These examiners engaged with stakeholders both virtually and in person and have conducted on-site fieldwork to help support their case findings.
In November 2024, BSI’s director, one assistant director, and one supervising fraud examiner participated as panelists at the Boston Chapter of the Association of Government Accountants’ “Many Faces of Fraud” event. The presentation provided an overview of BSI and the public benefit agencies and programs investigated by BSI (e.g., DTA, MassHealth, PCA, and EEC). The session concluded with a discussion of case examples that had been thoroughly investigated by BSI examiners.
Mentorship among BSI examiners remains a key priority for the unit. Examiners with expertise in interviewing, civil recovery and recoupment, report writing, and/or fieldwork consistently volunteer to support and guide their colleagues. This internal mentoring program has proven beneficial for both seasoned and newly hired examiners.
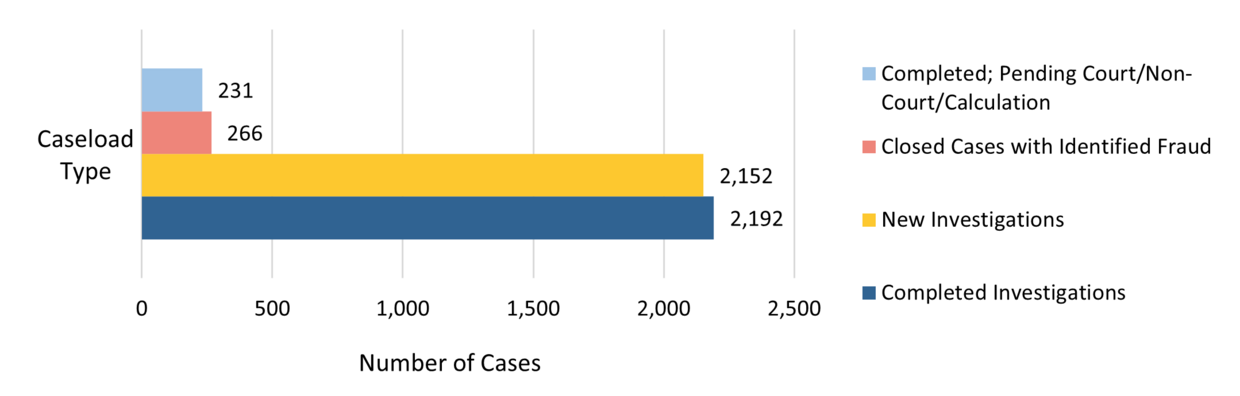
Figure 4. DTA Caseload for FY25*
* BSI’s DTA caseload for FY25 included SNAP, TAFDC, and EAEDC cases.
During FY25, FIU’s caseload included referrals generated through the PCA High Earner Project. The consistent finding in these cases that had identified fraud is that DTA cash and SNAP benefit recipients did not report their receipt of PCA income to DTA. Completed PCA cases with identified fraud were returned to DTA as IPVs for DTA’s administrative process and overpayment recovery. BSI civilly recovered $193,361 in public benefits issued to PCAs who did not report their PCA income to DTA.
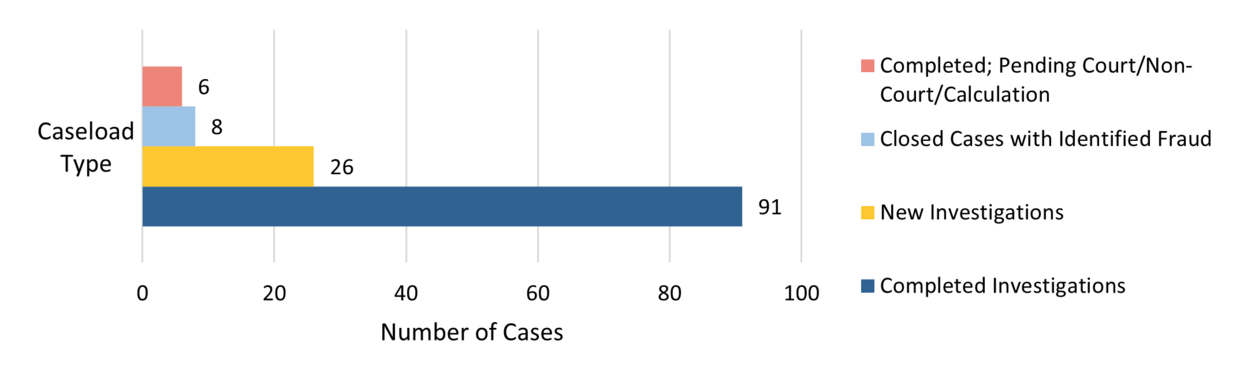
Figure 5. MassHealth Caseload for FY25*
* BSI’s MassHealth caseload for FY25 included cases related to healthcare benefits and PCAs.
During FY25, BSI case assignments included a variety of member benefit and PCA fraud cases. In addition to continuing to improve the referral intake and review process for joint investigations of PCA fraud-related cases, BSI and the Attorney General’s Office worked to improve the information-sharing process for PCA records and documentation. In PCA investigations, we make determinations regarding allegations of billing for services not provided, which often involves determining outside employment that would hinder or interfere with a PCA’s ability to perform PCA duties.
BSI also investigated whether PCAs who received other public benefits accurately reported their earned income to these public benefit programs. These investigations identified PCAs who did not report their PCA income and were overpaid for other public benefits.
EEC Caseload for FY25
Lastly, FIU completed one EEC investigation. Because individuals suspected of defrauding EEC often also receive other forms of public assistance, BSI routinely checks whether they receive other public assistance benefits and determines their reporting of household income and composition to other agencies. These supplemental investigations often discover additional errors or fraud in DTA and MassHealth public benefit programs.
As part of BSI’s expanding working relationship with EEC, BSI examiners participate in EEC’s administrative hearings under the Informal Fair Hearings Rules found in Section 10.11 of Title 606 of the Code of Massachusetts Regulations. EEC administrative hearings provide BSI examiners with the opportunity to explain their investigations and findings to EEC review officers.
Data Analytics Unit
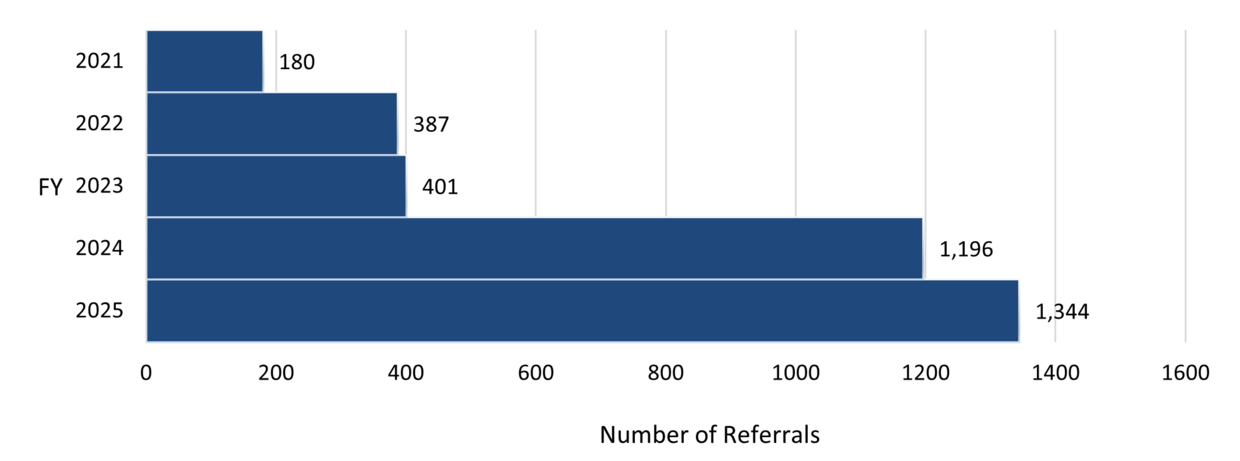
BSI’s DAU generated 1,344 referrals for CPU analysis in FY25. In the majority of these referrals, CPU found that PCAs did not accurately disclose their income to DTA and MassHealth, as required, while receiving public benefits.
DAU also identified MassHealth providers to refer for further action. The related analysis focused on improper billing associated with a variety of dental services. Other analyses conducted by DAU in FY25 focused on home health agency services, inpatient hospital services, long-term care, vision care services, PCA services, durable medical equipment, and chiropractor services. DAU also continued to receive referrals from BSI’s Public Assistance Fraud Hotline. During FY25, DAU received and analyzed seven provider referrals made through the hotline, some of which are ongoing as of the time of this report’s drafting.
DAU continued the operation and further development of its Analytical Support Services program. This program allows BSI examiners to use a suite of services designed to aid in the completion of data analysis tasks associated with their investigations. Some of these services include the creation of visualizations (e.g., maps, timelines, charts, and graphs) for presentation in court and other settings; custom findings reports for the analysis of financial, healthcare, and other data; network and social analysis; technical training; and optical character recognition (OCR) services. In FY25, DAU received, processed, and completed eight Analytical Support Services requests. Among the services provided, highlights include processing bank records through OCR and analyzing the output, creating visualizations from various data sources, analyzing PCA records, analyzing address records, and providing training assistance to other BSI units. By collaborating with examiners and completing these requests, DAU streamlined investigations by automating otherwise manual processes and summarizing vast amounts of information into a format easier to absorb.
During FY25, DAU continued to focus on the overall development of its OCR capabilities and the expansion of its use cases. DAU continued making strides in automating the processing of certain investigatory documents using OCR. Building on the work completed in FY24, which included the successful automated processing of financial records related to different bank account types from various financial institutions, DAU added two new bank account types to its library and successfully processed records associated with these institutions. These financial records are used solely in connection with BSI’s public benefit fraud investigations.
Additionally, DAU continued to make headway related to the automated processing of tax documents. DAU developed a summary of Form W-2, which passed multiple quality checks and a proof-of-concept stage. Additionally, DAU developed a summary of dependent information known as Schedule DI, which also passed multiple quality checks and a proof-of-concept stage. These advancements are critical to improving the efficiency and effectiveness of our work by automating BSI’s tax transcription process during fraud investigations.18 DAU also continued to make progress related to the automated processing of PCA timesheets. During FY25, DAU regularly processed the timesheets for one fiscal intermediary (FI),19 Tempus Unlimited Inc.,20 without issue.
Lastly, DAU began development on use cases related to the automated processing of handwritten documents. The expansion of OCR capabilities in these areas will enhance DAU’s ability to provide support to BSI examiners and their investigations. Indeed, DAU’s continued efforts to enhance and further develop the Analytical Support Services program have expedited the investigative process and streamlined certain operational functions within BSI. By using these services, examiners and other BSI units have decreased investigatory time by reducing or eliminating manual processes. Additionally, these services provide BSI with additional options in how information is processed, summarized, and presented during the investigative process.
DAU continues to support multiple state and federal partners through joint investigative work, in addition to accepting referrals for investigation and creating and sending referrals to the appropriate entities. For example, DAU is collaborating with federal partners, including the US Department of Health and Human Services’ Office of the Inspector General on an ongoing analysis related to services provided within both the Medicaid and Medicare programs.
Figure 6. DAU-Generated Referrals, by FY
Other BSI News
During FY25, BSI’s training team, comprised of staff members from all BSI units, continued identifying staff training needs; created informative and engaging trainings, presentations, and job aids; and effectively led training sessions for all BSI staff members. The training team continues to refresh BSI’s training content—which consists of multiple presentations, job aids, and learning templates—to reflect up-to-date federal poverty limits and any updated benefit program information. Onboarding materials serve as useful guides and remain available for all BSI staff members to reference.
In September 2024, BSI issued an updated policy manual with the training team’s assistance. As this update was the first since 2012, the manual is now aligned with BSI’s current investigatory process and includes commonly used terms, applications, and systems, as well as reporting requirements.
BSI initiated 41 repayment agreements and disqualification consent agreements (DCAs), totaling $1,657,549, during FY25. DCAs are agreements that subjects voluntarily sign to disqualify themselves from receiving further DTA and/or EEC benefits for a specific period of time because of IPVs. DCAs are required as part of the civil recovery agreement for DTA and EEC cases.
Although BSI’s new CMS project worked through its final phase, Phase III, during FY24, BSI continues to consider other system improvements that may enhance user friendliness, efficiency, and satisfaction. Potential system improvements include the ability to bulk expedite cases from certain workflows, fast-tracking to the assignment queue instead of a specific examiner or assistant director, and a separate list for cases in the calculation phase.
| Date published: | January 30, 2026 |
|---|